Drinking alcohol while taking diabetes meds isn’t just a bad idea-it can be dangerous. For people managing diabetes with insulin, sulfonylureas, or metformin, alcohol doesn’t just add empty calories. It interferes with your body’s ability to keep blood sugar stable, and it can push your liver into overdrive until it breaks down. The result? Low blood sugar that sneaks up hours after your last drink, or worse-liver damage that builds up silently over time.
Why Alcohol Makes Your Blood Sugar Drop
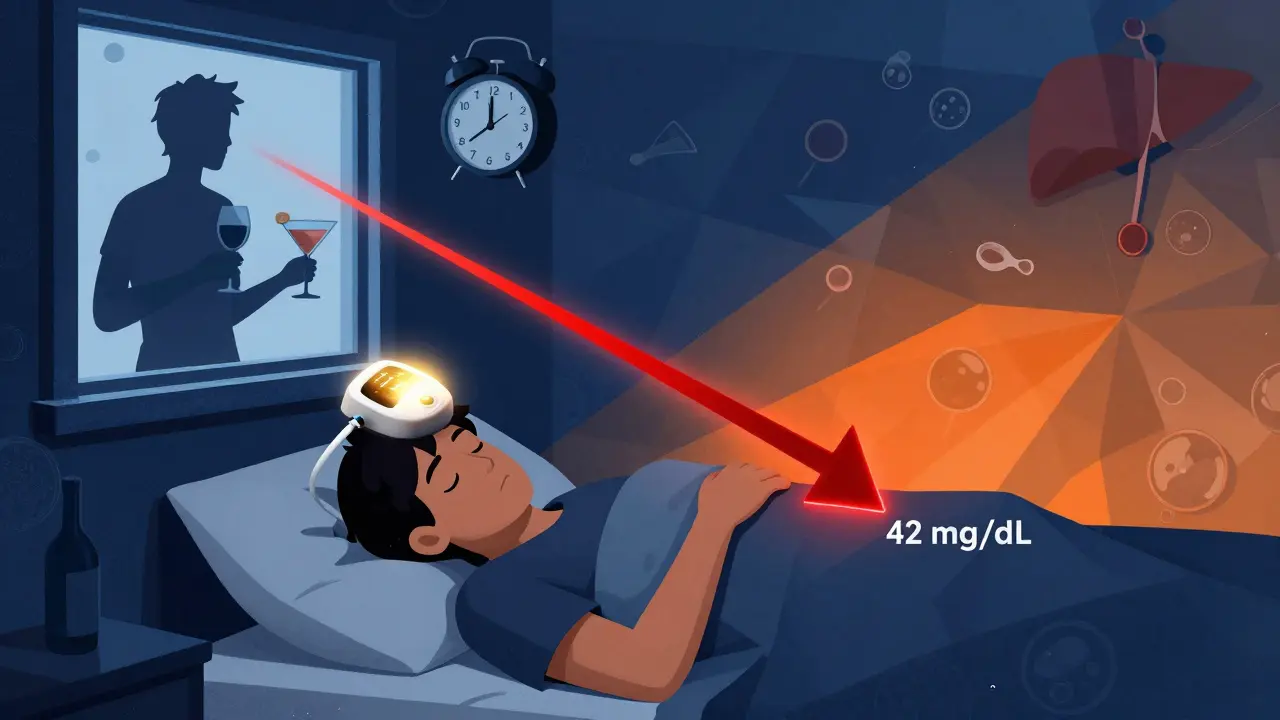
Your liver does two big jobs at once: it stores sugar when you’re full and releases it when you’re hungry. But when alcohol enters your system, your liver drops everything else to deal with it. Alcohol is toxic, and your body treats it like an emergency. So instead of releasing glucose to keep your blood sugar steady, your liver focuses on breaking down the alcohol. That’s when blood sugar crashes. This isn’t just a theory. The American Diabetes Association says hypoglycemia is the #1 risk when drinking with diabetes meds, especially insulin and sulfonylureas like glipizide or glyburide. These drugs push your pancreas to make more insulin. Alcohol blocks your liver’s ability to compensate. So you get a double hit: too much insulin in your blood and not enough sugar coming out of your liver. And here’s the scary part: symptoms of low blood sugar-dizziness, confusion, slurred speech, sweating, weakness-look exactly like being drunk. If you pass out after a few drinks, your friends might think you’re just wasted. They won’t realize you’re having a medical emergency. That’s why so many people with diabetes end up in the ER after drinking. Worse, the drop can happen hours later. You might go to bed with a normal reading, wake up at 3 a.m. with a pounding headache, shaky hands, and a heart racing. That’s delayed hypoglycemia. It’s common after drinking without food, especially if you exercised earlier in the day. Your liver is still busy cleaning up alcohol while your muscles are still sucking up glucose from the night before.How Metformin and Alcohol Stress Your Liver
Metformin is one of the most common diabetes pills. It helps your body use insulin better and doesn’t usually cause low blood sugar on its own. But when you mix it with alcohol, things get risky. Both metformin and alcohol are processed by the liver. When you drink, your liver has to handle the alcohol first. That means metformin sticks around longer than it should. This raises the chance of lactic acidosis-a rare but deadly condition where lactic acid builds up in your blood. It’s not common, but it’s more likely if you drink heavily, have kidney problems, or are dehydrated. Even if you don’t develop lactic acidosis, the combo can wreck your liver over time. Alcohol causes fatty liver, inflammation, and scarring. Metformin already puts mild stress on the liver. Together? That stress multiplies. Studies show people with type 2 diabetes who drink regularly have higher rates of liver enzyme spikes, which signal damage. And the side effects? They overlap. Nausea, stomach pain, vomiting, gas, and loss of appetite are common with metformin. Alcohol makes them worse. You might think you’re just getting sick from a bad meal, but it could be the combo of your pill and your drink.Which Diabetes Meds Are Riskiest With Alcohol?
Not all diabetes meds react the same way with alcohol. Here’s the breakdown:- Insulin and sulfonylureas: Highest risk. These directly lower blood sugar. Alcohol blocks the liver’s backup system. A single drink can trigger a dangerous drop.
- Metformin: Moderate risk. Doesn’t cause low blood sugar alone, but with alcohol, it increases chances of lactic acidosis and liver strain.
- SGLT2 inhibitors (like dapagliflozin, empagliflozin): Moderate risk. These make you pee out sugar, which can lead to dehydration. Alcohol is a diuretic too. Together, you’re at higher risk for low blood pressure and kidney stress.
- DPP-4 inhibitors (like sitagliptin): Low risk. These don’t cause hypoglycemia on their own, and alcohol doesn’t worsen them much.
- GLP-1 agonists (like semaglutide): Low to moderate risk. They slow digestion, so alcohol might hit slower-but nausea and vomiting can still get worse.
If you’re on insulin or sulfonylureas, you need to be extra careful. Even one drink without food can be risky. If you’re on metformin, occasional drinking might be okay-but only if your liver is healthy and you never drink on an empty stomach.
What You Should Do If You Drink
If you choose to drink, here’s how to stay safe:- Never drink on an empty stomach. Always eat a meal or snack with carbs before and while drinking. Think whole grain bread, fruit, or a small bowl of oatmeal.
- Choose low-sugar drinks. Avoid sweet cocktails, regular soda mixers, and dessert wines. Stick to light beer, dry wine, or spirits with soda water and lime.
- Limit how much you drink. Stick to one drink for women, two for men. More than that? You’re increasing risk fast. Heavy drinking (5+ drinks a day for men, 4+ for women) is dangerous for anyone with diabetes.
- Check your blood sugar before, during, and after. Test before you drink. Test every 1-2 hours while drinking. Test again before bed. If your reading is below 100 mg/dL, eat a snack.
- Set alarms. If you drink at night, set a phone alarm for 2 a.m. to check your sugar. Many people have lows while asleep.
- Wear medical ID. Make sure people around you know you have diabetes. A bracelet or phone alert could save your life if you pass out.
- Talk to your doctor. Ask if your specific meds are safe with alcohol. Some people need to avoid it completely.
What Experts Are Seeing Now
New tech is helping people manage this risk. Continuous glucose monitors (CGMs) like the Dexcom G7 and FreeStyle Libre 3 show trends over time. If your sugar drops suddenly after a drink, the graph will flag it. You can see patterns: “Every time I have two glasses of wine, I crash at 2 a.m.” That’s data you can use to change your habits. The American Diabetes Association updated its guidelines in 2023 to say there’s no one-size-fits-all rule. It’s all about your meds, your liver, your history of low blood sugar, and your drinking habits. Someone with fatty liver disease and frequent lows should probably skip alcohol. Someone with stable numbers and no liver issues might be fine with an occasional drink. But here’s the problem: most doctors don’t ask. A 2021 study found only 43% of primary care doctors bring up alcohol with their diabetic patients. That’s a huge gap. You need to start the conversation.
Real Stories From People Living With This
On diabetes forums, people share stories that sound like horror stories:- A 58-year-old man took his evening metformin, had two beers with dinner, and woke up at 4 a.m. with a blood sugar of 42 mg/dL. He had to call 911.
- A woman on insulin drank a glass of wine at a friend’s birthday party, didn’t test her sugar, and passed out. Her friend thought she was drunk-until she noticed the insulin pump on her arm.
- A man with type 2 diabetes drank three cocktails over two hours, didn’t eat, and didn’t check his sugar. He went into a coma. He survived, but now he avoids alcohol completely.
These aren’t rare cases. They’re common. And they’re preventable.
Bottom Line: It’s Not About Willpower-It’s About Biology
You don’t have to quit alcohol forever. But you need to treat it like a medication. It interacts with your body in ways you can’t control. Your liver can’t multitask. Your brain can’t tell the difference between intoxication and low blood sugar. Your meds don’t pause when you drink. If you’re unsure, don’t guess. Test your blood sugar. Talk to your doctor. Listen to your body. And if you’ve ever woken up scared because your sugar was too low after drinking-you already know the answer.Can I drink alcohol if I have type 2 diabetes and take metformin?
Yes, but with major limits. Occasional drinking (one drink for women, two for men) is usually okay if you eat food first and don’t drink often. But alcohol increases the risk of lactic acidosis, a rare but dangerous condition. It also makes metformin side effects like nausea and stomach pain worse. Never drink on an empty stomach, and avoid heavy drinking. Talk to your doctor if you have liver or kidney issues.
Why does alcohol cause low blood sugar in people with diabetes?
Your liver has to choose: detoxify alcohol or release glucose. When you drink, it prioritizes alcohol. That means it stops releasing sugar into your blood. If you’re on insulin or sulfonylureas, your body is already lowering blood sugar. Without liver backup, your sugar can crash-sometimes hours after your last drink.
How can I tell if I’m having hypoglycemia or just drunk?
You can’t always tell. Symptoms like confusion, dizziness, slurred speech, and sweating are the same. That’s why checking your blood sugar is the only reliable way. If you’re unsure, test. If your reading is below 70 mg/dL, treat it as low blood sugar-even if you think you’re just buzzed.
What drinks are safest for people with diabetes?
Choose low-sugar, low-carb options: light beer, dry red or white wine, or spirits (vodka, gin, whiskey) mixed with soda water and lime. Avoid sugary mixers like juice, tonic water, or soda. These spike your blood sugar first, then crash it later when the alcohol kicks in.
Should I avoid alcohol completely if I take insulin?
Many people on insulin are advised to avoid alcohol, but it’s not always required. If you’re careful-eat before drinking, test often, stick to one drink, and never drink alone-it can be done. But if you’ve had low blood sugar episodes before, or if you have trouble recognizing symptoms, it’s safer to skip it. Talk to your diabetes care team about your personal risk.
Can alcohol damage my liver if I have diabetes?
Yes, and it’s worse if you’re on metformin. Both alcohol and metformin stress the liver. Regular drinking can lead to fatty liver, inflammation, or even cirrhosis. People with diabetes already have higher rates of liver disease. Adding alcohol speeds up the damage. Get your liver checked if you drink regularly-even if you feel fine.
What should I do if I pass out after drinking?
If someone with diabetes passes out after drinking, assume it’s low blood sugar. Give them a glucagon injection if available. If not, call 911 immediately. Do not give them food, drink, or anything by mouth-they could choke. Never assume they’re just drunk. Time matters.



so i just had a glass of wine with dinner and my cgm went from 110 to 68 in 90 minutes. i thought i was just tired. turns out my liver was like 'nope, alcohol first, sugar later, maybe never.' now i get why my doctor looks at me like i'm a walking emergency.
February 25also, typo: 'liver' not 'live'... i mean, i know i'm not a doctor but come on.
Erin Pinheiro